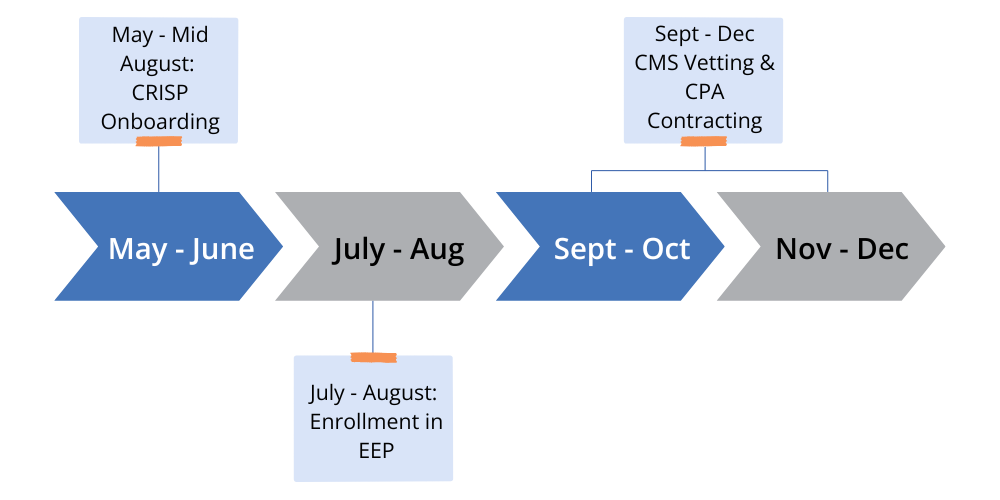
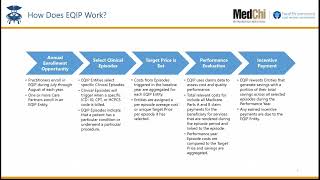
EQIP Introduction Policy Guide – PY5 – this document will cover the overarching goals of the program, the program structure and key policy components critical for participation
EQIP Specifications and Methodology PY5 – this document is a comprehensive reference on the methodology and implementation of the program
EQIP PY5 Episode Playbook – This is a catalog of all PY5 episodes inclusive of episode definitions, episode lengths, and trigger codes.
EQIP Eligible Episodes PY5 Slide Deck – This is a listing of all of the available episodes you could participate in for Performance Year 5.